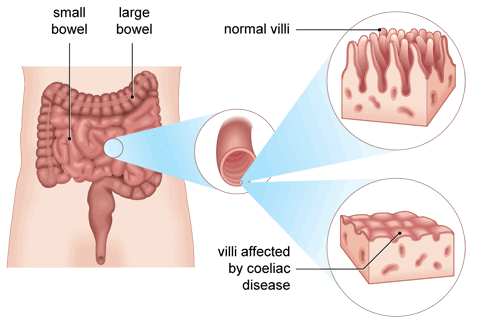
In the landscape of gastrointestinal diseases, coeliac disease has emerged from obscurity to occupy centre stage as a significant public health concern. It is a chronic autoimmune disorder triggered by gluten—a protein found in wheat, barley, and rye—in genetically predisposed individuals. On consuming gluten, the immune system mistakenly attacks the lining of the small intestine, leading to inflammation, villous atrophy, and impaired nutrient absorption.
While once thought to be rare in India, coeliac disease is now increasingly diagnosed, especially in regions where wheat is a dietary staple. North India, in particular, reports a growing number of confirmed cases. However, many still remain undiagnosed or misdiagnosed, often due to the disease’s broad clinical spectrum and lack of awareness among both healthcare providers and the general public.
The expanding clinical spectrum
Traditionally, coeliac disease was associated with classical gastrointestinal symptoms—chronic diarrhea, abdominal distension, weight loss, and failure to thrive in children. But medical understanding has significantly evolved.
Today, it is known that coeliac disease can present with:
- Atypical symptoms: fatigue, iron-deficiency anemia, short stature, delayed puberty, infertility, recurrent miscarriages, and osteoporosis.
- Extraintestinal manifestations: dermatitis herpetiformis (a chronic itchy skin rash), neurological disturbances, and liver enzyme abnormalities.
- Silent or subclinical disease: where the intestinal mucosa is damaged but the patient experiences minimal or no symptoms.
The age of presentation can range from early childhood to late adulthood, and the disease may even remain dormant for years before triggering symptoms due to stress, infection, pregnancy, or surgery.
Diagnosis: A prudent and precise approach

With the broadening phenotype comes the need for a structured diagnostic pathway. One of the most critical aspects in managing coeliac disease is establishing the correct diagnosis before initiating treatment. Unfortunately, this step is often bypassed, leading to confusion and misinformation.
Serological tests such as tTG-IgA (tissue transglutaminase antibody), and Anti-endomysial antibodies (EMA) are the first-line tools for screening. However, these tests must be done while the patient is on a gluten-containing diet, as antibody levels fall on a gluten-free diet (GFD), leading to false negatives.
Despite the high sensitivity and specificity of these tests, the gold standard for diagnosing coeliac disease remains upper gastrointestinal endoscopy with duodenal biopsy, where characteristic features such as villous atrophy, crypt hyperplasia, and increased intraepithelial lymphocytes can be seen.
This step is crucial because coeliac disease requires lifelong treatment. Initiating a GFD without biopsy confirmation may lead to diagnostic uncertainty. Later, if such individuals consume gluten and feel fine, they may erroneously believe they “outgrew” the disease. It is important to underline that coeliac disease cannot be outgrown. It is a lifelong autoimmune condition. If symptoms resolve without damage on biopsy, the initial diagnosis was likely incorrect.
In children with very high antibody titers and classical symptoms, recent guidelines (such as those from ESPGHAN) allow a biopsy-free diagnosis—but only under strict criteria.
Genetic testing for HLA-DQ2 or DQ8 may be helpful in ambiguous cases or when patients are already on a GFD. However, their absence virtually rules out coeliac disease, while their presence only indicates genetic susceptibility.
Management: beyond just avoiding bread

Once diagnosed, the cornerstone of management is a strict, lifelong gluten-free diet. No medications are currently approved to cure or reverse coeliac disease. Avoiding gluten allows the intestinal lining to heal and prevents complications.
However, maintaining strict dietary compliance is challenging, especially in India where:
- Wheat is a staple.
- Gluten-free food is expensive or hard to find.
- Food labels often do not declare gluten content.
- Cross-contamination is common in kitchens and restaurants.

Moreover, gluten is hidden in many places—soups, sauces, gravies, processed foods, cosmetics, and even medications. Even a small amount of gluten (less than 50 mg/day) can cause mucosal damage. Thus, compliance requires vigilance.
A trained dietitian is essential to guide patients through:
- Reading labels.
- Identifying hidden sources of gluten.
- Planning a balanced, nutritious GFD.
- Preventing deficiencies in iron, calcium, vitamin D, B12, and folate.
Regular follow-up with the physician and dietitian is important to monitor compliance, recovery, and nutritional status.
The risk of non-compliance and long-term complications
Patients who do not adhere to a GFD are at risk of:
- Persistent or worsening symptoms.
- Growth failure or delayed development in children.
- Nutrient deficiencies (anemia, osteoporosis, vitamin/mineral loss).
- Increased risk of intestinal lymphoma, particularly enteropathy-associated T-cell lymphoma (EATL).
- Other autoimmune disorders like type 1 diabetes, thyroiditis, and liver disease.
This underlines the importance of early diagnosis, education, and support systems to ensure sustained compliance.
Public health implications and the road ahead

India is currently undergoing a nutrition and diagnostic transition. With increased availability of diagnostic tests, better awareness, and growing access to information, more cases of coeliac disease are being identified. However, the true burden is still underestimated.
Here’s what’s needed:
- Awareness Campaigns: Educating parents, teachers, and healthcare providers about atypical signs of coeliac disease.
- Inclusion in National Health Programs: Especially under school health check-ups and adolescent health initiatives.
- Improved Food Labeling Regulations: To clearly declare gluten content.
- Subsidized Gluten-Free Products: Especially in school meal programs for diagnosed children.
- Training Programs for Dieticians: To specialize in coeliac and allergy nutrition.
- Support Groups and Advocacy Platforms: To help families and individuals with coeliac disease share knowledge and cope better.
Conclusion

Coeliac disease may be silent, but its impact can be profound. It is not a dietary fad, nor is it a transient intolerance. It is a lifelong autoimmune disease that demands medical precision, patient discipline, and societal support.
With proper diagnosis, dietary adherence, and regular monitoring, individuals with coeliac disease can lead healthy, fulfilling lives. But the key lies in recognition, education, and compliance—not just for the patients, but also for the community at large.

