Pain is an unpleasant sensory and emotional experience. It is associated with actual or potential tissue damage. Most painful experiences can be classified into two main categories – acute pain like a fractured bone, toothache, and insect bite or post-operative pain which usually lasts a short duration till the injury gets healed and chronic pain which lasts longer say for 3-6 months or maybe more due to chronic conditions like due to arthritis, nerve damage, or persistent injuries.
The perception of pain is subjective. Different people react to or tolerate pain differently. Management of pain may include medications (such as analgesics, anti-inflammatories, or opioids), physical therapy, occupational therapy, psychological interventions (such as cognitive-behavioural therapy or relaxation techniques), or complementary therapies (such as acupuncture or massage). The idea behind all this is to alleviate pain, improve function, and enhance the overall well-being of the individual.
Here are ten most painful diseases and conditions that are known to cause significant pain to people suffering from them:
Complex Regional Pain Syndrome (CRPS)

Complex Regional Pain Syndrome (CRPS), also known as reflex sympathetic dystrophy (RSD), is a chronic ailment that causes severe, continuous and prolonged pain. CRPS invariably starts in the hand, or foot, and also spreads to other parts of the body over time. The exact cause of CRPS is not known, but it is clear that it occurs after an injury or trauma in the affected limb.
Symptoms: The symptoms of CRPS generally include:
- Intense pain, burning, throbbing, or shooting sensation
- Swelling and changes in skin temperature
- Changes in skin colour and texture
- Stiffness, decreased mobility, and muscle weakness in the affected limb.
- Increased sensitivity to touch
- Changes in hair and nail growth
Diagnosis – The diagnosis of CRPS can be made after clinical evaluation of the symptoms and exclusion of other possible causes. There is no definitive cure for CRPS, but treatment can manage pain, improve function, and enhance the quality of life.
Treatment – CRPS is a debilitating condition that affects a person’s daily life and well-being. Treatment may include medications, physical therapy, occupational therapy, sympathetic nerve blocks, spinal cord stimulation, and psychological support.
Fibromyalgia

Fibromyalgia is a chronic disorder caused by a combination of genetic, environmental, and psychological factors. It is more common in women than men.
Symptoms: Symptoms of Fibromyalgia include musculoskeletal pain, fatigue, sleep disturbances, and tenderness in different parts of the body. The primary symptom of fibromyalgia often described as a deep, persistent ache, is chronic pain in the muscles, joints, and soft tissues throughout the body. People with fibromyalgia often experience persistent fatigue, even after getting adequate sleep. Other common symptoms include:
- fatigue,
- insomnia, sleep apnea, or restless legs syndrome
- difficulty in concentration, memory loss, and ‘blurred’ thinking, often referred to as “fibro fog.”
- tenderness or pain in the neck, shoulders, chest, hips, and knees when touched
- Migraines or tension headaches, abdominal pain, bloating,
- constipation,
- irritable bowel syndrome (IBS),
- increased sensitivity to light, noise, odours, and temperature changes
Diagnosis – Fibromyalgia is not easy to diagnose because there are no specific laboratory tests or imaging studies that can confirm it. The diagnosis depends on the evaluation of symptoms, medical history, and the presence of widespread pain and tender points.
Treatment – There is no cure for fibromyalgia. The best option to manage the pain, improve the quality of life, and enhance overall well-being may involve a combination of medications like pain relievers, antidepressants, and sleep aids, along with lifestyle changes, physical therapy, exercise, stress management techniques, and counselling according to specific symptoms and needs of the patient.
Trigeminal Neuralgia

Trigeminal neuralgia (TN) is a chronic pain condition that affects the trigeminal nerve, one of the largest nerves in the head. This results in severe, sudden, and recurring facial pain while eating or speaking. The trigeminal nerve is responsible for transmitting sensations from the face to the brain. The pain usually lasts for a few seconds or a few minutes. There are two types of trigeminal neuralgia: classic trigeminal neuralgia (known as Type 1) and symptomatic trigeminal neuralgia (known as Type 2). Classic TN is idiopathic, meaning the cause is unknown, while symptomatic TN is usually associated with an underlying condition such as multiple sclerosis or a structural abnormality.
Symptoms: Trigeminal neuralgia attacks can be triggered by normal activities like eating, speaking, or touching the face, as well as exposure to cold air. The pain is limited to one side of the face and commonly affects the lower part of the face, including the jaw, lips, and cheek. The symptoms of trigeminal neuralgia can include:
- Excruciating, sudden, and sharp facial pain like an electric shock or burning. The pain usually affects one side of the face and in specific areas, such as the lips, jaw, cheek, or eyes.
- Pain in the affected facial area that gets triggered by normal daily activities like eating, drinking, speaking, brushing teeth, or even a light touch. Exposure to cold air, or activities like smiling or yawning, may also trigger the pain
- Sudden, unpredictable episodes or attacks can last from a few seconds to a couple of minutes. These episodes can be frequent and may occur in clusters, followed by periods of remission where no pain is experienced.
- Pain in only one side of the face. It is rare for trigeminal neuralgia to affect both sides simultaneously.
- Absence of other symptoms: Unlike other facial pain conditions, trigeminal neuralgia usually does not cause numbness, tingling, or muscle weakness in the face. The pain is the primary symptom.
Diagnosis: Trigeminal neuralgia is usually diagnosed after a thorough examination of symptoms, medical history, and neurological examination. Sometimes doctors may prescribe a magnetic resonance imaging (MRI) test to rule out other causes of facial pain.
Treatment: Treatment for trigeminal neuralgia aims to reduce pain and improve the patient’s quality of life. Medications are often the first line of treatment. In some cases where medications are not effective or have intolerable side effects, nerve blocks, nerve ablation procedures, or surgery may be considered. Surgical intervention is advised in severe cases or when conservative treatments fail to provide relief. Some surgical options include microvascular decompression (MVD), radiofrequency ablation, and stereotactic radiosurgery.
Shingles (Herpes Zoster)
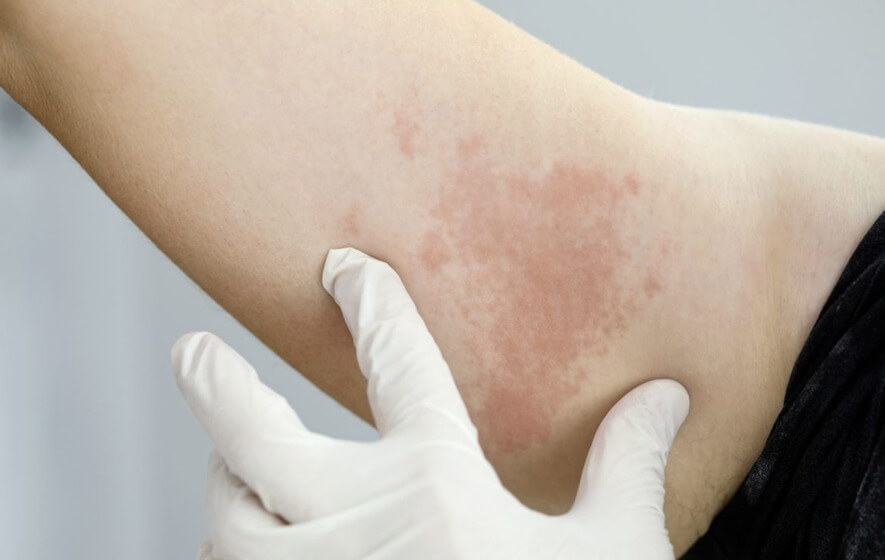
Shingles, also known as herpes zoster, is an infection caused by the varicella-zoster virus—the same virus that causes chickenpox. The infection causes a painful rash typically on one side of the body. After a person recovers from chickenpox, the virus can remain dormant in the nerve tissues near the spinal cord and reactivate later in life, leading to shingles. While most cases of shingles are cured without complications, some individuals may experience postherpetic neuralgia (PHN), which is persistent nerve pain that continues even after the rash heals. Other potential complications include bacterial skin infections, vision or hearing problems, and neurological issues if the virus affects the nerves in the head. Even though Shingles are not infectious or communicable a person suffering from shingles can transmit the varicella-zoster virus to someone who has never had chickenpox, leading to the development of chickenpox, if not shingles. The risk of developing shingles increases with age and is more common in individuals with a weakened immune system due to cancer, HIV, organ transplantation etc. Stress and trauma can also reactivate the virus. Vaccination is the most effective way to prevent shingles. The shingles vaccine, also known as the herpes zoster vaccine, is recommended for individuals aged 50 and older, including those who have previously had shingles.
Symptoms- The first sign of shingles is a painful rash that appears as a band or cluster of red, fluid-filled blisters. The rash is usually localized to one side of the body and follows the path of a specific nerve. Before the rash develops, individuals may experience pain, tingling, or burning sensations in the affected area.
Treatment — Antiviral medications are commonly prescribed to help shorten the duration of the shingles outbreak, reduce the severity of symptoms, and decrease the risk of complications. Pain management techniques, including over-the-counter or prescription pain relievers, may be recommended to alleviate discomfort.
Pancreatitis

Pancreatitis is a condition characterized by inflammation of the pancreas, an organ located behind the stomach that produces digestive enzymes and hormones like insulin. Inflammation of the pancreas can cause severe abdominal pain, often accompanied by nausea and vomiting. Pancreatitis can be acute meaning short-term, sudden and severe inflammation of the pancreas or chronic which means long-term inflammation of the pancreas that usually develops after repeated episodes of acute pancreatitis. Both forms have different causes and clinical presentations.
The most common cause of acute pancreatitis is gallstones or excessive alcohol consumption. Other causes include certain medications, infections, trauma, and high levels of triglycerides in the blood. Chronic pancreatitis is often associated with prolonged alcohol abuse, genetic predisposition, cystic fibrosis, and certain autoimmune conditions.
Symptoms- Symptoms of acute pancreatitis include severe abdominal pain, usually in the upper abdomen, that may radiate to the back, nausea, vomiting, fever, and a rapid pulse. Symptoms of chronic pancreatitis can include recurring abdominal pain, weight loss, diarrhoea, oily or fatty stools, nausea, and vomiting.
Diagnosis: Pancreatitis can be diagnosed by examination of physical symptoms, medical history, and diagnostic tests. Blood tests may reveal elevated levels of pancreatic enzymes (amylase and lipase). Imaging studies like ultrasound, computed tomography (CT) scan, or magnetic resonance imaging (MRI) can help visualize the pancreas and detect signs of inflammation or structural abnormalities.
Treatment: Treatment for pancreatitis depends on its severity. In acute pancreatitis, the goal is to relieve symptoms, manage pain, prevent complications, and allow the pancreas to heal. This often involves hospitalization, fasting, intravenous fluids, pain medications, and sometimes antibiotics. In chronic pancreatitis, treatment focuses on pain management, addressing complications (such as malnutrition or diabetes), and addressing the underlying cause, such as alcohol cessation or surgical interventions in some cases.
Cluster Headaches

Cluster headache is a type of intense headache primary headache that occur in cyclical patterns, causing severe, excruciating pain on one side of the head. The pain caused by cluster headaches is severe and focused around one eye, although it can radiate to the temple, forehead, face, or neck. It is also referred to as a “suicide headache” because of the severe pain. Cluster headaches are relatively rare, affecting less than 1% of the population.
Cluster headache attacks usually occur suddenly and reach their peak intensity within 5 to 10 minutes. They can last between 15 minutes and 3 hours and occur one to eight times a day. Cluster headaches occur in cycles or periods that can last for weeks or months. These periods are followed by remission periods during which the headaches do not occur. The cluster periods can be seasonal, with some individuals experiencing them at specific times of the year.
Symptoms: Cluster headaches are accompanied by autonomic symptoms, like redness and tearing of the affected eye, nasal congestion or runny nose on the affected side, drooping eyelid (ptosis), and sweating of the forehead or face. Restlessness, agitation, and difficulty sitting still are also common during an attack. Sometimes alcohol consumption, smoking, strong odours, high altitudes, certain foods, and changes in sleep patterns can trigger or precipitate cluster headache attacks.
Diagnosis: The diagnosis of cluster headaches is based on the individual’s symptoms and clinical evaluation. A healthcare professional will go through the medical history, physical examination, and some tests to rule out other possible causes of the symptoms.
Treatment: The treatment of cluster headaches aims to relieve pain during acute attacks, shorten the duration of the cluster period, and prevent future episodes. Acute treatment options may include high-flow oxygen therapy, triptans, or preventive medications to alleviate pain and reduce the frequency and intensity of cluster headaches. A healthcare professional, often a neurologist or headache specialist, is the best person to prescribe a specific management plan to address the challenges associated with cluster headaches.
Rheumatoid Arthritis
Rheumatoid arthritis (RA) is a chronic autoimmune disease that leads to chronic inflammation of the joints, causing joint pain and stiffness. Rheumatoid arthritis sometimes occurs when the immune system mistakenly attacks the body’s own healthy tissues, particularly the lining of the joints. The exact cause of RA is unknown, but genetic and environmental factors are believed to play a role. Rheumatoid arthritis can also affect other parts of the body leading to inflammation of the eyes (scleritis or uveitis), nodules under the skin, lung involvement, heart complications, and systemic inflammation that can impact other organs.
Symptoms – inflammation, pain, swelling, and stiffness in the joints, which can lead to joint deformity and loss of function over time. RA most commonly affects the hands, wrists, and feet, but it can also involve other joints and organs in the body. RA usually begins gradually, with symptoms that may include joint pain, swelling, stiffness (worse in the morning or after periods of inactivity), fatigue, and sickness. As the disease progresses, it can affect multiple joints symmetrically.
Diagnosis: A diagnosis of rheumatoid arthritis is typically made based on a combination of clinical evaluation, medical history, blood tests (such as rheumatoid factor and anti-cyclic citrullinated peptide antibodies), and imaging studies (such as X-rays or MRI) to assess joint damage.
Treatment: The treatment of rheumatoid arthritis involves reducing pain, inflammation, and joint damage, as well as improving function and quality of life. Treatment of rheumatoid arthritis largely depends upon the severity of the disease and may involve medications, physical therapy, regular exercise, and lifestyle modifications. Managing rheumatoid arthritis often requires comprehensive treatment by rheumatologists, physical therapists, occupational therapists, and pain specialists to meet the specific needs of each individual.
Currently, there is no cure for rheumatoid arthritis. Early diagnosis and appropriate management can help control symptoms, slow disease progression, and improve the quality of life of people suffering from rheumatoid arthritis.
Also Read: New age physiotherapy for treating back pain
Endometriosis

Endometriosis is a chronic condition in which tissue similar to the lining of the uterus grows on the ovaries, fallopian tubes, outer surface of the uterus, and other organs in the pelvic cavity outside the uterus, causing severe pelvic pain, especially during menstruation. Endometriosis can cause pain, infertility, and other complications. The exact cause of endometriosis is unknown, but several theories exist. Retrograde menstruation, where menstrual blood flows backwards into the pelvic cavity instead of leaving the body, is one possible explanation. Hormonal and immune system factors, genetic predisposition, and environmental factors may also contribute to the development of endometriosis.
Symptoms: The symptoms of endometriosis include infertility, fatigue and pelvic pain, before, during, or after menstruation. Other symptoms can include heavy or irregular menstrual periods, pain during intercourse, pain with bowel movements or urination during menstruation.
Diagnosis: Diagnosis of endometriosis typically involves a combination of a thorough medical history, physical examination, imaging tests (such as ultrasound), and, in some cases, laparoscopy to visualize and confirm the presence of endometriosis lesions.
Treatment: Treatment of endometriosis aims to manage symptoms, prevent the progression of the disease, and improve fertility. Treatment may involve pain medication, hormonal therapies (such as birth control pills), surgery to remove endometriotic lesions and in some cases, remove the uterus and ovaries. Fertility treatments may be necessary for women who have difficulty conceiving due to endometriosis. Managing endometriosis requires a multidisciplinary approach involving gynaecologists, reproductive endocrinologists, pain specialists, and mental health professionals. This approach ensures comprehensive care addressing the various aspects of the condition, including pain management, fertility concerns, and emotional well-being.
Kidney Stones
Kidney stones, also known as renal calculi, are hard mineral and salt deposits that form in the kidneys and can cause severe pain as they pass through the urinary tract. Kidney stones are typically formed when certain substances in the urine, such as calcium, oxalate, uric acid, or cystine, become concentrated and crystallize, forming solid masses. Various factors, including dehydration, medical conditions, dietary factors, and genetic predisposition, can contribute to stone formation. Kidney stones can vary in size and shape, ranging from as small as a grain of sand to as large as a golf ball. Kidney stones can cause severe pain when they move through the urinary tract.
Symptoms: The most common symptom of kidney stones is severe pain, which can occur in the back, side, abdomen, or groin area. The pain is often described as sharp and intermittent, and it may come in waves. Other symptoms can include blood in the urine (hematuria), frequent urination, urgency to urinate, cloudy or foul-smelling urine, and discomfort during urination.
Diagnosis: Diagnosis of kidney stones usually involves a combination of medical history, physical examination, urine tests, and imaging studies (such as X-rays, ultrasound, or CT scans) to determine the size, location, and composition of the stones.
Treatment: Treatment for kidney stones depends on factors such as the size, location, and composition of the stones, as well as the severity of symptoms. Small stones may pass out of the body through urine with increased fluid intake and pain management. Medications may be prescribed to help with pain and facilitate stone passage. For larger stones or those causing significant symptoms, treatment options can include extracorporeal shock wave lithotripsy (ESWL), ureteroscopy, percutaneous nephrolithotomy (PCNL), or rarely, open surgery.
There are a few preventive measures that can help reduce the formation of kidney stones. These include drinking plenty of fluids to maintain good urine output, adopting a balanced diet low in salt and animal protein, and following medical advice regarding dietary modifications.
Bone Cancer
Bone cancer refers to malignant tumours that develop within the bone, causing localized pain that can be severe, particularly as cancer progresses. There are several types of bone cancer, including osteosarcoma, Ewing sarcoma, and chondrosarcoma, each with its own characteristics and treatment. Bone cancer can also occur as a result of metastasis from other primary cancers, spreading to the bones from other organs.
Osteosarcoma is the most common type of bone cancer. Both Osteosarcoma and Ewing sarcoma affect children and young adults, while Chondrosarcoma mainly affects adults. Other less common types include chordoma, fibrosarcoma, and malignant giant cell tumours.
The prognosis or diagnosis of bone cancer can vary depending on the type and stage of cancer, as well as individual factors. Early detection and appropriate treatment can improve outcomes. Early diagnosis can make a big difference in the tumour’s response to treatment, the presence of metastasis, and the overall health of the individual.
Symptoms: The symptoms of bone cancer can vary depending on the location, size, and stage of the tumour. Common signs and symptoms may include persistent bone pain, swelling or a lump over the affected area, bone fractures without significant trauma, fatigue, weight loss, and, in advanced cases, anaemia and other systemic symptoms.
Diagnosis: Diagnosing bone cancer involves a combination of medical history evaluation, physical examination, imaging tests (such as X-rays, CT scans, MRI, or bone scans), and biopsy to examine the affected bone tissue and determine whether it is cancerous.
Treatment: Treatment for bone cancer depends on various factors, including the type, size, location, and stage of the tumour, as well as the overall health of the individual. Treatment options may involve surgery to remove the tumour, radiation therapy to target and destroy cancer cells, chemotherapy to kill cancer cells throughout the body, and in some cases, targeted therapies or immunotherapy. Treatment plans are often developed by a multidisciplinary team of healthcare professionals specializing in oncology, orthopaedics, and radiation therapy.
Conclusion

This is not an exhaustive list, and there are many other disease conditions that can cause excruciating and unbearable pain. If you or someone you know is experiencing persistent or severe pain, it is essential to seek medical attention for an accurate diagnosis and appropriate treatment.

